AXS Vecta 0.071–0.074 Inch Aspiration Catheters for Mechanical Thrombectomy: Case Series and Literature Review
Article information
Abstract
Aspiration catheters are widely used for thrombectomy either alone or in combination with a stent-retriever, with a distal inner diameter and trackability keys to their success. In an illustrative case series, we report our clinical experience with AXS Vecta (Stryker Neurovascular, Fremont, CA, USA), available in both 0.071-inch and 0.074-inch distal inner diameters, including the first 2 Vecta 74 cases reported. A literature review on AXS Vecta is also provided. In our series, 9 thrombectomies were performed (Vecta 71: 2 M1, 5 M2 occlusions; Vecta 74: 1 M1 and 1 ICA-terminus occlusion). The AXS Vecta was successfully delivered to the target site in all cases. In 7 of 9 cases, the catheter was delivered over a Tenzing 7 delivery catheter (Route 92 Medical, San Mateo, CA, USA). For 2 of 9 combination approach cases, Vecta was delivered using the stent-retriever wire as a rail. The median improvement in NIHSS score during hospitalization was 9 (IQR 5–12). Successful mTICI 2C or 3 recanalization was achieved in 8 of 9 (89%) patients after a median 2 (IQR 1–2) passes. Our median groin-to-reperfusion time was 23 (IQR 12.5–32) minutes, with no procedural complications. Two previous clinical studies of a total of 29 patients treated with Vecta 71 reported successful mTICI 2b–3 recanalization in 89–90% of cases. The Median groin-to-reperfusion time was 30 minutes. Complications were seen in 2 of 29 (6.9%) cases (vessel perforation and/or intracerebral hemorrhage). These data support the efficacy, deliverability, and safety of AXS Vecta for mechanical thrombectomy.
INTRODUCTION
Several randomized clinical trials have shown the significant benefits of mechanical thrombectomy (MT) over medical management in patients presenting with acute stroke with large vessel occlusions (LVOs) with absent or small core infarcts [1-7]. The vast majority of thrombectomies in these trials were performed using stent-retriever (SR) devices. Since then, several alternative thrombectomy techniques have gained acceptance.
Aspiration thrombectomy using the a direct aspiration first pass technique (ADAPT) is an efficient and cost-effective means of rapidly restoring perfusion in LVO stroke patients [8-10]. The ADAPT technique relies on delivering an aspiration catheter to the proximal aspect of the embolus and applying suction to the catheter to aspirate the embolus. The proposed advantages of the ADAPT technique over SRs include: a faster time to first pass, less need to pass microwires and delivery microcatheters into more distal artery branches beyond the embolus, decreased damage to the endothelial wall [11], decreased vessel traction during device removal, decreased clot disruption, and decreased cost [12]. Two randomized trials, the contact aspiration vs. stent-retriever for successful revascularization (ASTER) [8] and a comparison of direct aspiration vs. stent-retriever as a first approach (COMPASS) [9] trials, compared SR and ADAPT techniques as firstline thrombectomy options. In both trials, SR and ADAPT techniques achieved similar rates of successful reperfusion and 90-day functional independence [8,9]. In addition, cost savings were achieved in the ADAPT cohort. These 2 randomized control trial (RCT), alongside a meta-analysis of 6 RCTs (871 patients), demonstrated that Solitaire SR and aspiration catheters have equal safety, providing sufficient evidence to recommend ADAPT as a reasonable first-line endovascular therapy (EVT) approach [13].
SRs may also be used in combination with aspiration catheters to maximize clot retrieval forces at both the clot face and along its length. This combination technique is also widely utilized [14,15], and may be advantageous in tortuous intracranial anatomy by optimizing the angle at which the SR is withdrawn (“line of force”) and avoiding undesirable traction on the artery itself. Initial studies evaluating the combination technique have reported high recanalization rates (88% thrombolysis in cerebral ischemia [TICI] 2B or 3), a low number of passes, and good functional outcomes [15-24].
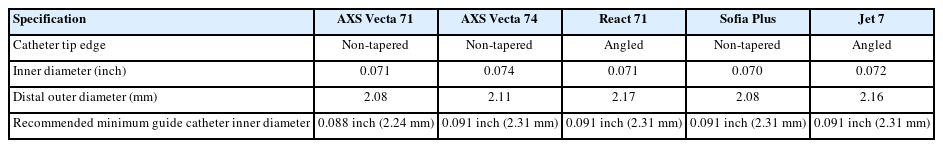
Aspiration catheter design improvements over time have focused on larger inner diameter (ID) at the tip (for increased suction force), and improved catheter trackability (or deliverability) through tortuous anatomy. Use of larger catheters with ADAPT (0.070 inch or greater) may be associated with increased aspiration flow rates, first pass effect, faster recanalization, reduced procedure time, and better reperfusion rates [25,26], compared to less sizes than 0.070. Currently, available aspiration catheter ID now range between 0.035 inches and up to 0.074 inches [27-31]. The AXS Vecta 71 and AXS Vecta 74 (Stryker Neurovascular, Fremont, CA, USA) aspiration catheters were recently approved for thrombectomy, with an ID of 0.071 inches and 0.074 inches, respectively. The Vecta 071 can be delivered through a 0.088-inch guide catheter or larger. The slightly larger Vecta 74 must be delivered through a 0.091-inch ID guide catheter (e.g., AXS INFINITY LSTM PLUS Long Sheath; Stryker Neurovascular) or larger. Herein, we report our initial experience in 9 patients with AXS Vecta 71 and 74 for MT using aspiration and combination techniques for the purpose of assessing their safety and efficacy. In addition, we review current literature on AXS Vecta in acute ischemic stroke MT.
METHODS
Case Series
Using a prospective collected institutional stroke patient database, we retrospectively reviewed medical records of consecutive patients with stroke who underwent MT at our center with AXS Vecta 71 or 74 catheters between September 16, 2018, and May 16, 2022. All patients who received MT had evidence of LVO on computed tomography (CT) angiogram. Patient selection for thrombectomy was based on the most recent American Heart Association Guidelines [13]. We confirm that this study was an observational, minimal-risk study, and no patient informed consent was required as the research did not include any patient identifying information, per the California Pacific Medical Center (CPMC) Research Institute Policy. This study was approved by the CPMC Institutional Review Board (approved protocol 2.16.17).
Study Variables
Collected data for each patient included age, sex, race, stroke risk factors (hypertension, diabetes, hyperlipidemia, atrial fibrillation, smoking), time of symptom onset, stroke severity on arrival measured by the National Institutes of Health Stroke Scale (NIHSS), baseline functional status as measured by modified Ranking Scale (mRS) before symptom onset, intravenous (IV) thrombolytic use, and time of groin puncture. Patient imaging included admission CT. Admission CT angiography was reviewed to document the admission Alberta stroke program early CT score (ASPECTS) and the location of the vascular occlusion. Angiography, procedure reports, and follow-up CT or magnetic resonance imaging (MRI) were reviewed to document outcome variables including number of passes, reperfusion time, procedural complications, rate of symptomatic intracerebral hemorrhage (sICH) transformation, and discharge NIHSS. Procedural complications and final reperfusion score using the modified TICI (mTICI) grading scale were used to document pre-thrombectomy occlusion and post-thrombectomy revascularization. sICH was defined using the European Australian Cooperative Acute Stroke Study II definition as any intracerebral hemorrhage on any posttreatment imaging after the start of tissue plasminogen activator with an increase of ≥4 points in NIHSS score [32].
Technique
Thrombectomy procedures were performed by 1 of 3 experienced neurointerventionists (JDE, WTK, and FS). In brief, vascular access was obtained using a 9-French femoral sheath. A large guide catheter, (e.g., Infinity Long Sheath [Stryler Neurovascular], was advanced into the distal cervical segment of the internal carotid artery. In this series, for combination SR+local aspiration (cases 1–2), the AXS Vecta catheters were delivered in a coaxial fashion over a Prowler Plus (Cordis Neurovascular, Miami, FL, USA) microcatheter and a 0.014-inch Synchro2 Standard microwire (Boston Scientific Corp., Marlborough, MA, USA). In these combination technique cases, the stent-retriever was deployed first, and then the aspiration catheter was brought to the face of the clot (or to the M1 segment, if presenting as an M2 occlusion) [14,15] using the SR wire as a rail. The ADAPT technique has been described in previous reports [33]. For aspiration thrombectomy (ADAPT) cases 3–9, the Vecta catheter was delivered using a shelf-reducing Tenzing 7 delivery catheter (Route 92 Medical, San Mateo, CA, USA) without a leading microwire. The delivery catheter was then removed, and aspiration was applied with a vacuum aspiration pump for 3–5 minutes before pulling the aspiration catheter back until free blood return was observed in the aspiration tubing. If no free flow was seen in the tubing, the catheter was completely removed from the patient.
Statistical Analyses
Descriptive statistics were used to report patient demographics and clinical characteristics of the included patients. The analysis was conducted using SPSS v25 (IBM Corp., Armonk, NY, USA).
Literature Review
An extensive online literature search was performed to identify other studies reporting the use of AXS Vecta aspiration catheters in MT. Online databases available through our institution, including PubMed and Medline, were searched using keywords: “Vecta” and “Thrombectomy” and “Stroke”. We reviewed angiographic data from both English and non-English studies. Study variables include median age, sex, baseline non-contrast CT ASPECTS, IV thrombolytic use, occlusion site, procedural technique, device, mean/median number of passes, mean/median procedural time, successful recanalization according to modified treatment in cerebral ischemia score (mTICI 2b–3, >50% reperfusion of the target vessel) after the first pass, complete recanalization (mTICI 2c–3) within a single attempt (first-pass effect), overall procedural success (mTICI 2b–3 and 2c–3), rate of complications, and functional outcomes (improvement in NIHSS at either post-procedure day 1 or at discharge).
RESULTS
Case Series
Nine consecutive patients underwent thrombectomy using the AXS Vecta catheters at our institution during the study period. Table 1 summarizes the characteristics of the included patients. The mean age was 65 (standard deviation 19.9) years, 4 of 9 were female, 4 of 9 were Caucasian, 3 of 9 were Hispanic, and 2 of 9 were Asian. The most common stroke risk factor was hypertension (in 7 of 9) followed by atrial fibrillation (in 3 of 9), and hyperlipidemia (in 3 of 9). The baseline mRS was in the range 0–1 for all patients, except 1 that had a baseline mRS of 3. The median ASPECTS was 7 (interquartile range [IQR] 5–9). The median last known well to groin puncture time was 409 (IQR 260–500) minutes.
Seven of 9 cases were performed using the Vecta 71 catheter and 2 of 9 were performed with the Vecta 74 aspiration catheter (Fig. 1). The ADAPT technique was utilized in 7 of 9 cases, with the catheter delivered over a Tenzing 7 delivery catheter (Route 92 Medical) (Fig. 1). For 2 of 9 combination approach cases, the Vecta was delivered using the SR wire as a rail.
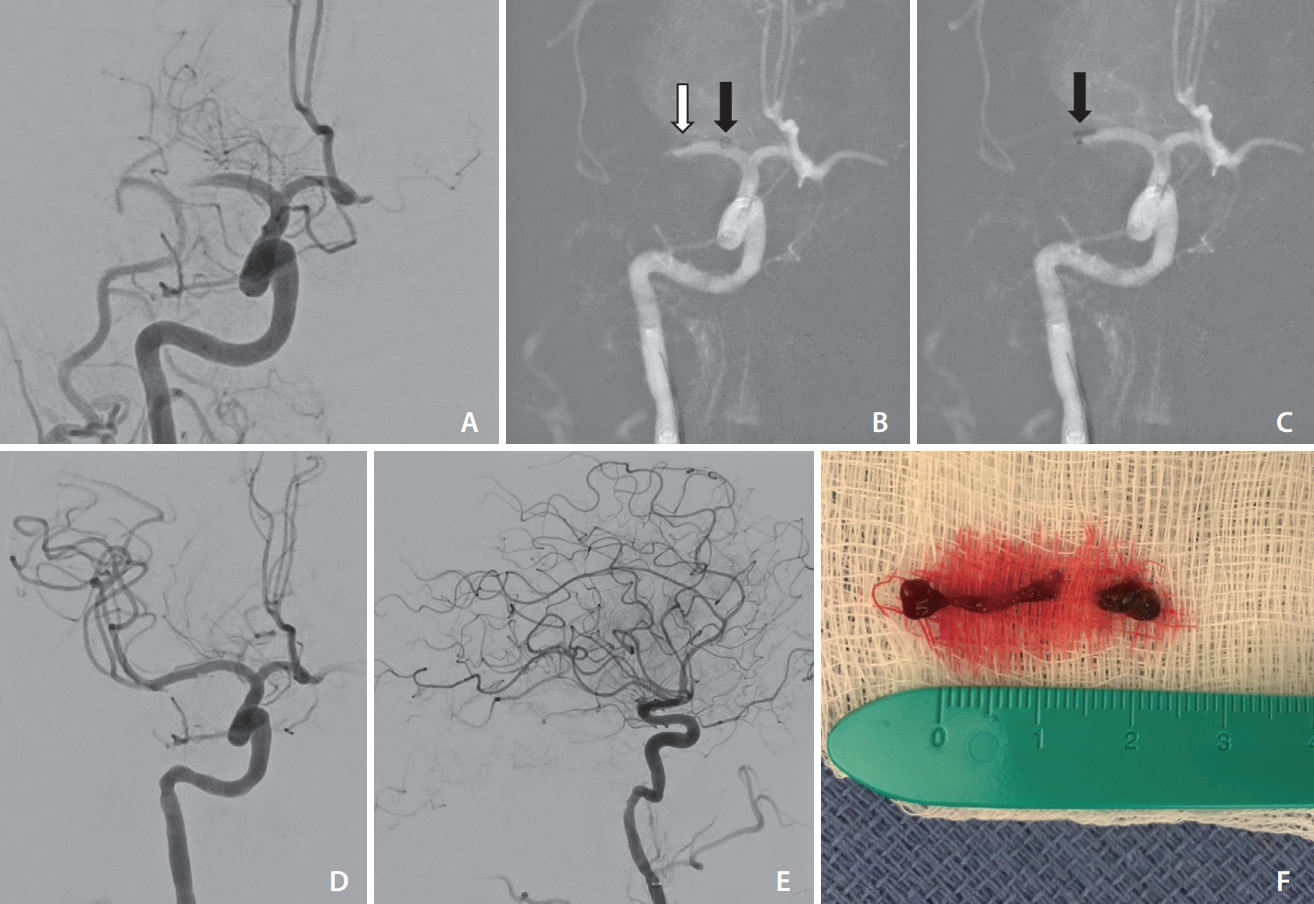
(A) Initial cerebral angiogram showing an occlusion at the M1 segment of the right middle cerebral artery. (B, C) The delivery of the AXS Vecta 74 catheter (Stryker Neurovascular, Fremont, CA, USA) (black arrows) to the occlusion site over a Tenzing 7 delivery catheter (Route 92 Medical, San Mateo, CA, USA) (white arrow). (D, E) Final cerebral angiography imaging showing successful recanalization (mTICI score 3). (F) Photo of retrieved thrombus. mTICI, modified thrombolysis in cerebral ischemia score.
Successful reperfusion (mTICI ≥2B) was achieved after a median of 2 passes (IQR 1–2). The median groin puncture to reperfusion time was 23 (IQR 12.5–32) minutes. The AXS Vecta catheters demonstrated excellent navigability and tractability, which aided in achieving mTICI 2C or 3 in all cases except case 8. Case 8 had a final mTICI of 0. Although the Vecta 71 achieved initial full reperfusion, the middle cerebral artery (MCA) quickly re-occluded due to underlying an underlying atherosclerotic plaque. Rescue therapy with IV GPIIB/IIIA inhibitor +/– stenting was not performed due to the presence of a nonspecific hyperdense pontine lesion on the initial pre-procedure CT (differential diagnosis included acute hemorrhage, hemorrhagic neoplasm, or cavernous malformation) and risk subsequent life-threatening hemorrhage. Unfortunately, by the time an MRI was performed to further characterize the pontine lesion, a large core infarct had developed in the right MCA territory. The median improvement in NIHSS at discharge, excluding 1 patient that died during hospitalization from pneumonia, was 9 (IQR 5–12).
No vessel perforation, dissection, or other procedural complications were identified during or after any of the procedures. None of the patients had sICH following the procedure. One patient died post-procedure due to respiratory failure.
Literature Review
Two clinical studies (with a total of 29 cases) [31,34] who underwent MT with AXS Vecta 71 catheters were identified in the literature and reviewed. Demographics, procedural data, and outcomes are presented in Table 2 and are compared to the current study. No studies were found that reported on the use of Vecta 74.
Gross et al. [31]. reported on 19 patients who underwent thrombectomy using Vecta 71 on the first pass as part of a larger study (a total of 59 patients) comparing the efficacy and safety with 2 other aspiration catheters (React 71 [Medtronic, Irvine, CA, USA] and 0.072-inch Jet 7 [Penumbra, Alameda, CA, USA]). [31] Clinically, the mean improvement in NIHSS score on the first post-treatment day (8±7.0) for patients in the Vecta group was not different in comparison with the other 2 groups (P=0.16). Overall, similar angiographic results were noted using all 3 0.071-inch and 0.072-inch large-bore aspiration catheters (final mTICI 2b–3 achieved in 92% of cases overall: 95% with React 71, 89% with Jet 7, and 89% with Vecta 71). Excluding empiric stentriever usage, the aspiration catheter could be delivered to the clot without needing a stentriever in 87% of cases overall: 100% with React 71, 93% with Vecta 71, and 43% with Jet 7 (P=0.002), indicating that React 71 and Vecta 71 tracked more reliably to the clot over a microcatheter as compared with the Jet 7 catheter. In addition, procedure-related complications (perforation or hemorrhage) were seen in 4 of 49 patients (8%): 1 of 21 React 71 cases, 2 of 19 Vecta 71 cases, and 1 of 19 Jet 7 cases. Procedural times were similar across groups. Of note, 12 of 49 (24%) patients died within the available follow-up period; this rate did not significantly differ between the 3 groups.
Almallouhi et al. [34] reported on 10 patients who underwent thrombectomy using Vecta 71 with the ADAPT technique. Nine out of 10 (90%) received IV tissue plasminogen activator before thrombectomy. The median ASPECTS was 7.5 (IQR 7–8.75). The median symptom onset to groin puncture time was 261.5 (IQR 252.25–303.25) minutes. Successful reperfusion (mTICI 2b or 3) was achieved with 1–3 aspiration attempts in all cases except for 1 case (4 aspiration attempts and stent-retriever attempts were unsuccessful due to underlying severe intracranial atherosclerosis). The authors were able to deliver the AXS Vecta to the target in 9 of 10 cases, except in 1 case where the AXS Vecta could not be advanced past the M1 because of the small caliber secondary to atherosclerosis. The median groin puncture to reperfusion time was 29.5 (IQR 14.25–53.25) minutes. None of the patients suffered sICH following the procedure.
DISCUSSION
Previously published data suggest that the Vecta 71 catheter can be used to perform rapid, effective, and safe MT [31,34]. Our series of patients treated with Vecta catheters resulted in successful revascularization in a similar proportion of cases as previously published studies (89%), using both ADAPT and the SR plus a local aspiration technique, without complications (Table 2). Clinical outcomes seen with Vecta 71 and 74 in our series were also similar to these previously published in Vecta 71 reports [31,34] (Table 2). The AXS Vecta catheter reached the clot in nearly every case across the studies. As reported by Gross et al. [31], Vecta 71 and React 71 tracked particularly better than Jet 7, as clot access in the Jet 7 group required a different use of alternate catheters (2 of 9 patients) or use of a SR as a rail (2 of 9 patients).
The median number of passes in our study, 2, was similar to prior reports, with similar first pass effect rates (42% vs. 33%). There was a higher proportion of proximal M2 occlusions in our study, 5 of 9 (56%) patients, compared to 0 patients with M2 occlusions in Gross et al. [31]. Almallouhi et al. [34] had 6 of 10 (60%) cases of M2 occlusions. MT of M2 occlusions requires anatomical considerations: the caliber of the M2 branch (such as a dominant inferior division M2 segment) must be large enough to accommodate a large bore aspiration catheter and the tortuosity and acuity of the angle of the M1 MCA bifurcation must permit a large bore aspiration catheter to take a turn without causing a dissection or perforation. As a result, the use of large bore aspiration catheters is limited to cases with a favorable anatomy.
The median groin-to-reperfusion time of 23 minutes in our study was more rapid than previously reported for Vecta 71 [31,34]. This is likely due to our use of a Tenzing 7 delivery catheter (Route 92 Medical), which significantly reduces the space between an inner microcatheter and outer aspiration catheter or ledge. This is especially important with the increasing caliber of aspiration catheters, which have a greater tendency to catch on the ophthalmic artery origin and have increased friction in tortuous anatomy. A ledge-reducing delivery catheter provides a more robust rail in the center of the vessel lumen. In an in vitro study, we previously showed that the Tenzing 7 is capable of delivering aspiration catheters to the proximal M1 in half the time compared to a leading microwire/microcatheter [35]. For similar reasons, such delivery catheters may also improve access to proximal M2 MCA occlusions (4 of 7 ADAPT cases in our series were proximal M2 occlusions). Ledge-reducing delivery catheters, such as the Tenzing 7 or AXS Offset (Stryker Neurovascular) [36] may also be less disruptive to the clot and less likely to induce thrombus fragmentation and distal embolization. When using the ADAPT technique as a first-line approach, difficulty may be encountered in delivering an aspiration catheter to a thrombo-embolus due to a number of factors, such as vascular tortuosity, intracranial atherosclerotic disease, small native vessel caliber, or ophthalmic artery origin anatomy. In such cases, the use of a stentriever anchoring technique may be considered. After stentriever deployment, the stentriever wire functions as a rail and is more centered in the vessel lumen compared to a 0.021–0.035 inch microcatheter, minimizing the ledge effect.
A number of physical properties contribute to the efficacy of a thrombectomy aspiration catheter: ID, navigability and trackability, kink and ovalization resistance, and catheter tip distensibility. A recent study compared the in vitro navigability and trackability of various large aspiration catheters when advancing over a microcatheter/microwire support system through a sinusoidal glass vascular anatomy model [37]. This study, however, included an older generation Cat 7 aspiration instead of the Vecta 71 catheter. The Cat 7 catheter uses a continuous nitinol round wire wind, while the Vecta catheter features a supportive braided proximal stainless steel coil shaft (for enhanced pushability) and a nitinol coil on the approximately distal 10.8 cm of the catheter (for enhanced flexibility and durability). These properties provide smoother catheter navigation with both a microcatheter/microwire and stentriever anchoring techniques. In our series, we were able to track the Vecta catheters to the target site in each case, as distally as the proximal M2 segment MCA, indicating that the Vecta 71 catheter can be navigated to this distal location in some cases. It is important, however, that operators using a catheter of this size for ADAPT recognize that in patients who have significant intracranial atherosclerotic disease, these catheters may be too large to maneuver to or through the M1 segment. Moreover, in some cases utilizing ADAPT as a first line approach, the combination of a stent-retriever and aspiration catheter may be necessary to retrieve emboli that are resistant to initial direct aspiration passes. Additional characteristics differentiate the Vecta from other available large bore aspiration catheters (Table 3) include a non-tapering distal tip, a low profile distal outer diameter (for 0.070–0.072 catheters), and an option to use a larger version (Vecta 74).
This is also the first report of 2 clinical cases of aspiration thrombectomy using the Vecta 74 catheter. Direct aspiration thrombectomy requires an aspiration force strong enough to successfully engage, engulf, and remove the thrombus. The ADAPT technique was initially described with aspiration catheters having a 0.054–0.060 inch ID[33]. In the ADAPT arm of the ASTER trial, aspiration catheters used included Penumbra ACE64 (65/174, 37%) or smaller catheters (5MAX, ACE60, Sofia) [8]. The COMPASS trial used the Penumbra ACE68 (57%, 76/134) or ACE64 (30%, 40/134). Neither trial included patients treated with 0.070 inch or larger distal ID catheters, however, since these were not yet commercially available. Since then, several studies comparing larger and smaller bore aspiration catheters have shown improved outcomes, shorter procedure times, and a lower likelihood of using additional devices without impacting complication rates with a larger bore [25,38]. This relates not only to increased suction force at clots with larger IDs, but also increased aspiration flow rate with decreasing catheter size to vessel diameter ratio [26]. Consequently, design and engineering improvements have permitted a trend in increasing catheter distal ID without clinically significant sacrifices in navigability, pushability, and durability in most instances [39]. The Vecta 74 represents a further step in this trend. This catheter shares the same design characteristics and materials as the Vecta 71, but with a slightly larger inner and outer diameter (see Table 3). The vendor states that this larger outer diameter of Vecta 74 requires the use of a slightly larger guide catheter, such as the Infinity LS Plus Long Sheath (Stryker Neurovascular), which has a 0.091 ID but still goes through an 8F vascular sheath.
Several other large bore aspiration catheters (0.070–0.074) are currently available from different vendors: React 68 and 71 (Medtronic, Minneapolis, MN, USA), Sofia Plus (Micro-Vention Terumo, Tustin, CA, USA), as well as Jet 7, and more recently RED72 (Penumbra). The construction of all of these catheters shows a high degree of similarity, with all catheters featuring the following: (1) inner polytetrafluoroethylene (or Teflon) liner; (2) hybrid reinforcement using a proximal braided coil (for pushability, torquability, and kink/ovalization resistance) and a distal non-braided coil (for flexibility through tortuous anatomy); (3) blended polymer jackets of varying/transitioning stiffness along the catheter shaft; and (4) outer hydrophilic coating (for reducing friction). Subtle specification differences between catheters exist (Table 3). Studies of clinical experience with these catheters has yielded similar rates of efficacy (reperfusion rates, number of passes, procedure times, outcomes), and safety (procedural complications) to AXS Vecta 71 [27,40-42]. There are no published clinical studies utilizing RED72 catheters at this time.
A recent in vitro study [43] compared the navigation performance in a glass phantom model mimicking tortuous vascular anatomy for the following different large bore aspiration catheters: Vecta 74, Cat 6, ACE 68, Jet 7 (Penumbra), React 68 and React 71 (Medtronic), and Sofia Plus (MicroVention Terumo, Tustin, CA, USA). Similar tracking forces were needed for Vecta 74 catheter advancement using unsupported advancement compared to other catheters. When tracking over a microcatheter/microwire or stentriever wire, however, slightly higher tracking force was needed for Vecta 74 compared to all other catheters except the ACE 68. To date, however, no in vitro study has compared tracking forces across different aspiration catheters when using a delivery assist catheter. Such delivery catheters, including Tenzing (Route 92 Medical), Offset (Stryker Neurovascular), and Wedge (MicroVention Terumo), will very likely reduce gaps in tracking forces between different aspiration catheters [35,36,44]. Further increases in aspiration catheter ID may be desirable from a suction force perspective. However, there are potential disadvantages as catheters become larger and begin to asymptotically approximate the caliber of the large artery itself, including increased friction in the artery and risk of endothelial damage leading to arterial vasospasm, dissection, and/or perforation.
This study is limited by a relatively small number of clinical studies of Vecta 71 catheters available for review and the absence of prior Vecta 74 clinical studies. Our case series is limited by the single-center design and the small sample size. Larger scale retrospective or prospective studies are necessary to confirm the initial findings and detect potential complications of using Vecta catheters. Future in vitro studies comparing aspiration catheters from different vendors should also include Vecta catheters and delivery assist catheters.
In this early experience with the Vecta 0.071–0.074 inch aspiration catheters, successful reperfusion was achieved in 89% of patients within a fast reperfusion time and without procedural complications, similar to prior reports. Larger studies are needed to confirm the findings and further assess the efficacy and safety of the Vecta 74 aspiration catheter.
Notes
Fund
None.
Ethics Statement
Ethics approval was obtained from the Institutional Review Board of California Pacific Medical Center (approved protocol 2.16.17). Due to the retrospective nature of the study, the need for patient informed consent was waived. As any information such as sex or age is not included, Informed consent for publication is not required.
Conflicts of Interest
FS reports consulting fees, grant, and honoraria from Stryker; consulting fees from Route 92 Medical; grant from MicroVention. WTK reports an equity interest in and consulting fees from Route 92 Medical, as well as consulting fees from Stryker. JDE reports an equity interest in and consulting fees from Route 92 Medical, as well as consulting fees from Stryker.
Author Contributions
Concept and design: FS. Analysis and interpretation: FS, WTK, and JDE. Data collection: FS and JDE. Writing the article: FS. Critical revision of the article: FS, WTK, and JDE. Final approval of the article: FS, WTK, and JDE. Statistical analysis: FS. Overall responsibility: FS.