|
 |
- Search
| Neurointervention > Volume 17(3); 2022 > Article |
|
Abstract
Notes
Ethics Statement
The Institutional Review Boards of Baylor Scott and White Health and Texas A&M University have waived the requirement for informed consent. The patient information has been anonymized.
Conflicts of Interest
The authors hereby declare that they have no relevant conflicts of interest to disclose. WSL is an investigator in the Medtronic (Dublin, Ireland) Embolization of the Middle Meningeal Artery With ONYXŌäó Liquid Embolic System for Subacute and Chronic Subdural Hematoma (EMBOLISE), but this patient was not part of the trial.
Author Contributions
Concept and design: AVPN, SRD, BL, and WSL. Analysis and interpretation: AVPN, SRD, BL, and WSL. Data collection: AVPN, SRD, BL, and WSL. Writing the article: AVPN, BL, and WSL. Critical revision of the article: AVPN, SRD, BL, and WSL. Final approval of the article: AVPN, SRD, BL, and WSL. Overall responsibility: WSL.
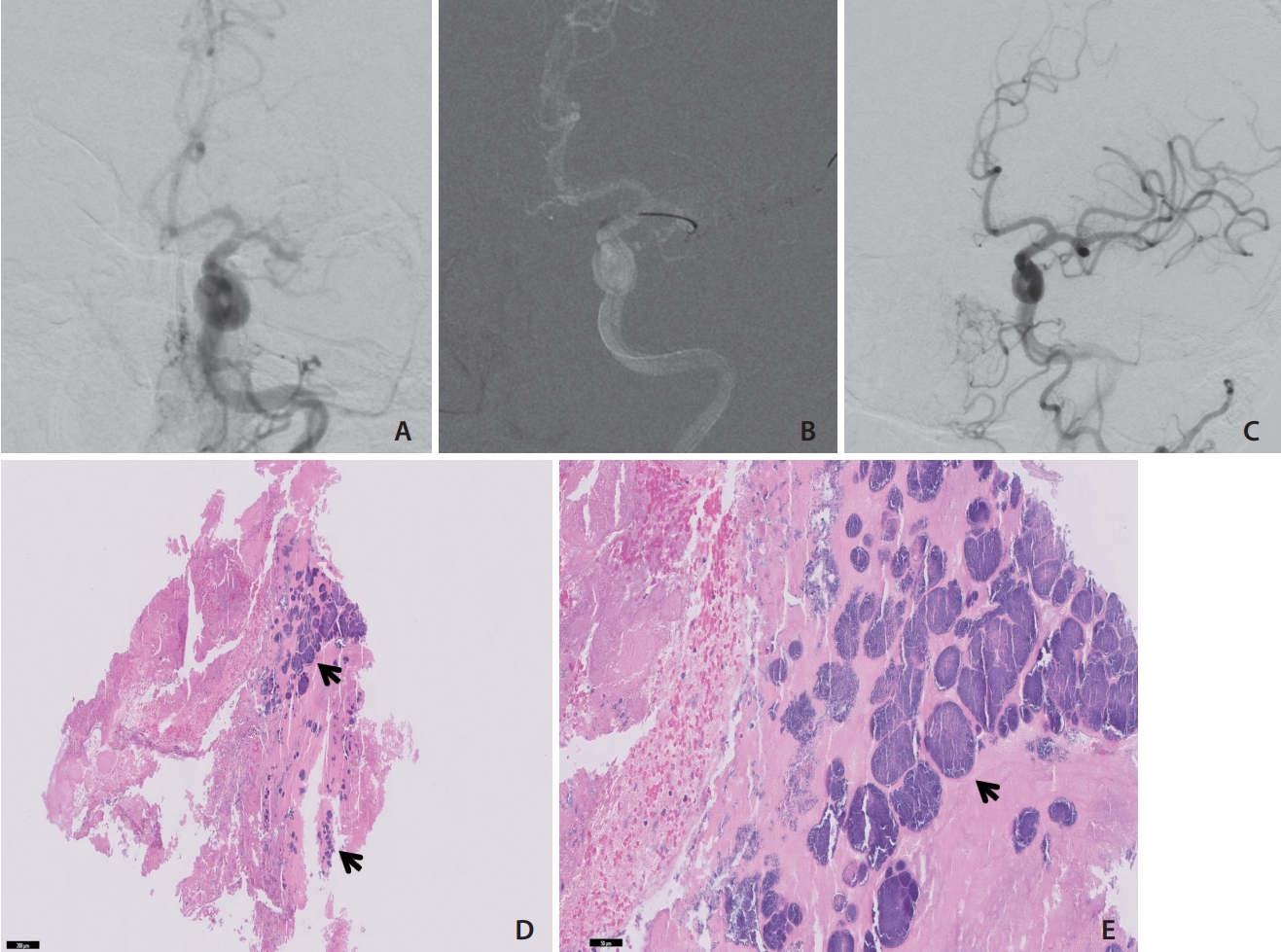
Fig.┬Ā1.